Leprosy Can be Well Treated
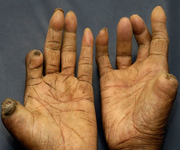
Leprosy (Hansen's disease) is categorized a contagious syndrome in which there is damage of skin, peripheral nerve injury, and progressive debilitation. This type of medical condition develops by infectivity with the bacteria Mycobacterium leprae.
In India, leprosy is found in many states and a community health problem where the number of registered cases (62% of the global burden) is 0.55 million. Statistical data indicated in 1997 that leprosy patients who had noticeable disability were 3.9% and victims with actual malformation due to leprosy were 1.49 million. It has been observed that many leprosy patients, who are recovered bacteriologically, still have some physical, emotional, psychological, social and economical problems.
The cases of leprosy differ from state to state. Overall whole country is under grip of this disease. When the bacteria of leprosy (Mycobacterium leprae) enter in body of person, the bacteria immediately begin to reproduce within the body. Leprosy symptoms appear after three to five years.
This period between becoming infected and the start of symptoms is the leprosy incubation period. Although the incubation period is usually between three and five years, it can vary from six months to several decades. Person who is infected with leprosy usually face problems in the skin and peripheral nerves. However, once a person starts experiencing symptoms, they can range in type and severity. Symptoms can also be different based on the type of leprosy that a person has.
It may be tuberculoid leprosy or lepromatous leprosy. Mycobacterium leprae which is responsible for leprosy, grow gradually and mainly harm the skin, nerves, and mucous membranes. It has been observed that in severe cases of leprosy, Mycobacterium leprae damage the testes, hands, feet, skin, peripheral nerves, front portion of the eyes, upper respiratory passages. Many scientists consider that leprosy spreads from person to person through infected respiratory droplets. It can be considered as one form of leprosy transmission but more than 50 percent of cases, the disease have no confirmed contact with an infected person. Other factors that are responsible for developing leprosy in a person are the extent of exposure, Genetics, Environmental conditions.
There are many forms of leprosy. Tuberculoid leprosy, known as paucibacillary leprosy, is the
less severe form of leprosy. Patient shows symptoms of light or
slightly red patches of skin that appear on the trunk or
extremities. This may be related with a decrease in light-touch
sensation in the area of the rash.
Tuberculoid leprosy, known as paucibacillary leprosy, is the
less severe form of leprosy. Patient shows symptoms of light or
slightly red patches of skin that appear on the trunk or
extremities. This may be related with a decrease in light-touch
sensation in the area of the rash.
Other tuberculoid leprosy symptoms are severe pain, muscle weakness, especially in the hands and feet, skin stiffness and dryness, loss of fingers and toes, eye problems, which lead to blindness, enlarged nerves, especially those around the elbow (ulnar nerve) and knee (peroneal nerve).
According medical professionals, all leprosy patients do not lose their fingers and toes. If patients visit doctor and get treatment at an early stage of disease, many of these symptoms can be prevented. Many tuberculoid patients recover with their immune system without benefit of treatment. Leprosy patients should avoid injury and infections to fingers or toes to prevent damage in these areas and take their medicines regularly to recover fast.
People must be fully aware of risk factors associated with leprosy. Generally, it has been seen that people who live within the same household as a person with leprosy patient who is not taking any treatment are increased risk of developing the disease. It is because there are genetic factors related to vulnerability or prolonged close contact. People must know that the partner is the least-at risk family member. There are people who are at the greatest risk of leprosy transmission such as parents of someone with leprosy, children leprosy patients. It is a known fact that leprosy cannot be spread from a mother to her unborn baby and people cannot get leprosy through sexual contact.
To diagnose leprosy, a physician asks numerous questions about the patient's symptoms, current medical conditions, and medications, among other things. To confirm leprosy in patients, the doctor will likely ask questions about: symptoms, current medical conditions, medications, travel history, family history of any medical conditions and possible exposure to someone with leprosy. During the exam, the doctor observes at the skin and other parts of the body for signs of leprosy.
If it is suspected that patient is suffering from leprosy, the
will recommend certain tests. The doctor can make a perfect
diagnosis of leprosy by doing a skin biopsy. For leprosy
patients, this skin biopsy will disclose a particular pathologic
pattern and demonstrate the specific red-staining bacteria.
There are other diseases which show common symptoms with
leprosy, including: Systemic lupus, erythematosus (lupus), Lupus
vulgaris, Sarcoidosis, Dermal leishmaniasis, yaws. Tests usually
confirm whether patient is having leprosy or not. Leprosy
diagnosis is delayed because it can resemble other skin
diseases.
Treatment of leprosy generally depends on the type of the disease. Doctors recommend antibiotics in all cases as is supportive care, which helps to lessen symptoms and complications. Multidrug therapy (MDT) is common treatment of the leprosy removal strategy as it cures patients, decreases the infection and prevents further transmission. MDT also prevents disabilities through early treatment. When treatment is given to leprosy patients, leprosy is categorized into two types.
The first one is Pauci-bacillary (PB) leprosy in which there are 1-5 skin lesions - schedule of two drugs - Rifampicin and Dapsone for 6 months. Secondly, Multi-bacillary(MB) leprosy in which there are greater than 5 skin lesions - schedule of three drugs - Rifampicin, Clofazimine and Dapsone for 12 months. The drugs are given in different blister packs for PB and MB leprosy and for Adults and Children in each type. These medicines are taken strictly as per doctor's recommendation. Any article or journal can give overview so that people can generate awareness and visit doctors immediately.
Medical science does not have any vaccine currently for the prevention of leprosy. Leprosy can be treated with medicines. It is advised to all populace that they should contact doctors whenever they notice any symptoms of leprosy. An early diagnosis may decrease associated symptoms and complications.
It is a fact that deterrence of leprosy is not possible, particularly where the disease is widespread but through great efforts, it can be controlled. To prevent this disease, people who live in the same family as a person with leprosy will require to be examined by a doctor. These examinations should be frequent annually for five years. It is important to know that the degree of natural immunity is high, and sometimes people do not require any preventative medicine.
Articles on Health
- Laparoscopic Surgery Advantages
- Laparoscopic Surgery History
- Laparoscopic surgery Procedures
- Limitations of traditional laparoscopic surgery
- New technologies for advance laparoscopic surgery
- Non-Robotic Laparoscopic Surgery
- Robotic Laparoscopic Surgery
- Causes and remedy for dark circles in females

- Harmful impact of mobile phone on unborn baby

- Maternal health care tips

- Rheumatoid Arthritis is Most Widespread in Female
- Periodontal ailment during Pregnancy
- Anemia is prevalent in Women
- Effect of Cell phone tower radiation on human health

- Current health scenario india
- Government health policies india
- Medical facilities india
- Hospital infrastructure india
- Shortage of Medical Professionals in India
- Quality standards indian hospitals
- Indian states health statistics
- Medical expenses india
- Hospitals in Ahmedabad
- Hospitals in Bangalore
- Hospitals in Chennai
- Hospitals in Cochin
- Hospitals in Delhi
- Hospitals in Hyderabad
- Hospitals in Kolkata
- Hospitals in Mumbai
- Hospitals in Pune
- Hospitals in Coimbatore
- Hospitals in Kochi
- Orthopaedics Hospitals in India
- Diabetology Hospitals in India
- Cardiology Hospitals in India
- Infertility Hospitals in India
- Neurology Hospitals in India
- Paediatrics Hospitals in India
- Nephrology Hospitals in India
- Oncology Hospitals in India
- Antiaging foods to improve skin

- Tips for Maintaining healthy bones
- Guidelines for preventing heart disease
- Tips to reduce eye strain while working on computer
- Mental health problems among elderly people
- Health problem of piles

- Health advices for air travel

- Dealing with Allergies
- Tips for Eyes Care
- Care for Crystal Clear Skin
- Tips For Healthy Hair
- Healthy Living is The Absolute Measure of Happiness
- Let Fragrance Rule Your Summer
- Most common vestibular disorder

- Osteoporosis Risk Factors
- Dengue

- Endocrine disorder

- Causes of liver damage
- Dry eye syndrome
- Kidney Stones
- Conjunctivitis: Irritating eye disease
- Anxiety Disorder
- Causes of Brain Damage
- Hepititis B
- Knowledge of Osteoarthritis
- Mental Illness
- Back Pain
- Sugar Addiction
- Diet Control Plans
- General Motors Diet Plan
- No Carbohydrate Diet
- One day Diet Plans
- Seven day diet Plans
- Vegetarian Diet
- Food for Health
- Genetically Modified Foods
- Healing Effects Of Fruits
- Vegetables That Heal
- Healing Effects Of Spices and Herbs
- Test your Stress Level
- Mantras for Relaxation & Stress free life
- Take walk For a healthy body and mind
- Squint is frequently observed in Children
- Consult-Doctor
- Free Handy Health Advice